Defination:-
pancreatitis is an acute inflammatory process of the pancreas and its caused by an inciting event which damages the pancreatic parenchyma, leading to a chain reaction.
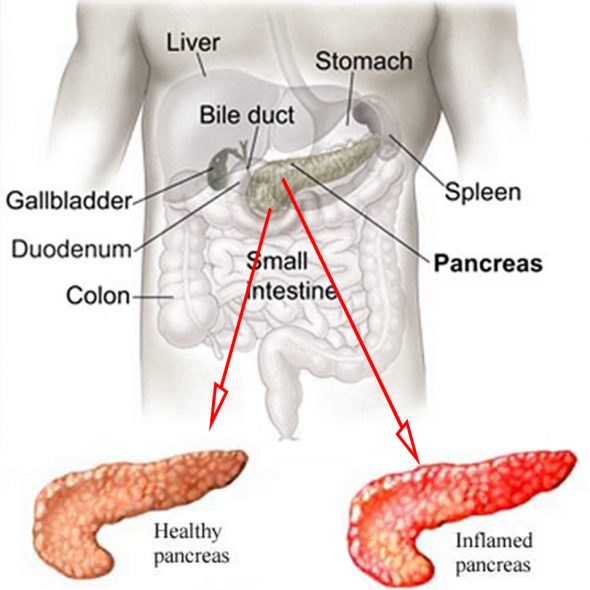
What are the different types of pancreatitis?
There are two types of pancreatitis: acute and chronic.
Acute pancreatitis
Acute pancreatitis is a temporary condition. It happens when your pancreas is attempting to recover from a minor, short-term injury. Most people with acute pancreatitis will recover completely in a few days with supportive care and home care.
Chronic pancreatitis
Chronic pancreatitis is a long-term, progressive condition. It doesn’t go away and gets worse over time. It happens when the injury or damage to your pancreas never stops. Chronic pancreatitis will eventually do lasting damage to your pancreas, although it may take many years.
What are the symptoms of pancreatitis?
The primary symptom of pancreatitis is abdominal pain.
Additional symptoms of acute pancreatitis may include:
- Nausea and vomiting.
- Fast heart rate.
- Fast, shallow breathing.
- Fever.
- Additional symptoms of chronic pancreatitis may include:
- Indigestion and pain after eating.
- Loss of appetite and unintended weight loss. Fatty poops that leave an oily film in the toilet.
What are the most common causes of pancreatitis?
The top two causes of pancreatitis are:
- Gallstones.
- Heavy drinking.
Other causes
- Infections, such as viruses.
- Autoimmune disease (autoimmune pancreatitis).
- Inherited gene mutations (hereditary pancreatitis).
- High blood triglyceride levels (hypertriglyceridemia).
- High blood calcium levels (hypercalcemia).
- Ischemia (reduced blood supply).
- Cancer.
- Traumatic injury to your pancreas.
- Certain medications that irritate the pancreas
How to diagnose?
Pancreatitis is diagnosed by
- physical exams
- blood tests (specifically high lipase or amylase levels)
- imaging studies like abdominal CT scans or ultrasounds
Key Diagnostic Methods:
Blood Tests: Elevated amylase and lipase (lipase more specific) are key indicators, along with checks for high blood sugar or fat levels.
Imaging Tests:
Abdominal Ultrasound: Primary tool to detect gallstones, a common cause of pancreatitis.
CT Scan: Assesses the severity, inflammation, and potential complications like fluid collections.
MRI/MRCP: Detailed imaging of the pancreas and bile ducts.
Endoscopic Ultrasound (EUS): A highly sensitive method used to find blockages or small stones.
Prevention of Pancreatitis:-
Although not all cases of acute pancreatitis can be prevented, the following lifestyle changes can reduce your risk:
Limit Alcohol Consumption: Excessive drinking is one of the leading causes of acute pancreatitis. Moderation is key to preventing alcohol-induced pancreatitis.
Maintain Healthy Triglyceride Levels: High levels of triglycerides in the blood can contribute to pancreatitis. Maintaining a healthy diet and lifestyle can help keep your triglyceride levels in check.
Eat a Balanced Diet: Eating a diet low in fats and high in fiber can promote good pancreatic health.
Seek Medical Care for Gallstones: If you have gallstones, seek medical advice early to prevent complications like pancreatitis.
Treatment:-
There is no specific medicine to treat pancreatitis. treatment begins with a hospital stay to manage symptoms and complications.
The following treatments are commonly recommended for pancreatitis.
Lifestyle changes
People with chronic pancreatitis will need to undergo some lifestyle changes. These will include:
Stopping alcohol consumption: Giving up drinking will help prevent further damage to the pancreas. It will also contribute significantly towards relieving the pain. Some people may need professional help to quit alcohol.
Stopping tobacco use: Smoking is not a cause of pancreatitis, but it can accelerate the progression of the disease.
Pain management
Treatment should not only focus on helping ease the pain symptoms, but also depression which is a common consequence of long-term pain.
Doctors will usually use a step-by-step approach, in which mild painkillers are prescribed, gradually becoming stronger until pain becomes manageable.
